Meet a difference maker…in health and wellbeing – John Civardi
7th April 2022
In this blog series, which is part of our recently launched Sustainability Hub, we’re speaking to chemical engineers across the world making a difference to make sustainable practices and products a reality and more accessible to all for the wider benefit of our society and globe.
Today on World Health Day (7 April 2022), John Civardi talks about his experience as a water engineer, and how water is being contaminated with pharmaceutical waste, which could lead to the development of drug-resistant bacteria. He also explains why it’s important for chemical engineers to help solve this issue for better treatment and cleaning of waterways, groundwater and other water sources to prevent future threats to humans, animals and the environment.

Name: John Civardi
Job title and organisation: Global Water and Wastewater Treatment Practice Leader, Mott MacDonald, USA
Bio: John is responsible for coordinating the implementation of best practice across Mott MacDonald’s 1,600-strong water and wastewater treatment practice area. He has a wide range of experience in water treatment, serving as project engineer or project manager for numerous surface water and groundwater treatment projects. John has also been responsible for the pilot testing, evaluation, design, and construction administration of water treatment systems throughout the US and has served as technical advisor on projects around the world.
He is also the co-author of the second edition of the Iron and Manganese Handbook published by the American Water Works Association and has recently written the manual on Ion Exchange for Drinking Water Treatment (also for the American Water Works Association).
Tell us about your career in the water sector and particularly with relation to emerging contaminants?
I have been working in the field for 36 years now and have gained experience with the use of a variety of processes, including adsorption clarifiers/filters; membranes; superpulsators; ballasted flocculation; granular activated carbon, ozone, and dissolved air flotation; as well as residuals processes for the likes of solids dewatering.
I have been responsible for the evaluation and design of systems to remove iron, manganese, volatile organic compounds, and radionuclides using treatment processes including air stripping, diffused bubble aeration, granular activated carbon, manganese greensand, ion exchange, membranes, and ultraviolet disinfection.
This experience has also enabled me to assist owners and operators to evaluate distribution system water quality. The need of many water and wastewater utilities to comply with the US Environmental Protection Agency (EPA) regulatory requirements of the Lead and Copper Rule, Disinfection By-products Rule, and Total Coliform Rule have occasionally resulted in compliance problems. I have assisted utility companies in resolving compliance problems through the development of sampling strategies, along with the design, construction, and operation of pipe loops to evaluate treatment changes.
This has also led to a passion for understanding emerging contaminants of concern. There is a lot of focus on developing strategies for climate change and climate resilience; however we cannot take our eye off risks associated with the likes of Perfluorinated Alkyl Substances (PFAS), endocrine disruptors, and we are also now seeing issues with these contaminants in our source water with the associated risk of passing these to our water network. These substances can potentially have adverse health impacts on the liver, immune system and fertility.

What is antimicrobial resistance and how is this affecting water contaminants and human health?
Antimicrobial resistance (AMR) is part of a broader set of issues we are seeing in the water sector with emerging contaminants.
AMR occurs when bacteria no longer respond to the antimicrobial agents, such as antibiotics and antifungals, that were designed to kill them.
Whilst AMR is not new, microorganisms such as bacteria and fungi have been developing resistance for millions of years as a natural evolutionary process (or survival of the fittest), we have accelerated this process through misuse of antimicrobials in human medicine and in farming, as well as the discharge of a host of polluting chemicals into our environment which – through a process called co-selection - make AMR more likely.
One way AMR can develop is when antimicrobial concentrations are too low to be fatal to the microorganism, allowing those with a beneficial trait to gain an advantage and to proliferate further. These resistant organisms can then spread through the water, environment and between animals and humans. When drug-resistant organisms spread in hospitals, the impact can be even more significant due to patients having weakened immune systems.
Globally, around 70% of antimicrobials are used in animal or fish farming and others still in arable farming (for wheat and barley). In farming, around two thirds of active compounds in antimicrobials pass out of an animal on defecation. The same happens with humans, in that much ends up in the waste system, compounded by indiscriminate flushing of unwanted antimicrobials down toilets (with wastewater treatment discharges often going into waterways or onto productive farmland).
Once resistance develops, there is potential for the resistant bacteria and genes to spread along multiple pathways, colonise and cause infections in people and animals. A key pathway in the spread of AMR and antibiotic residues is through rivers and waterways. This will ultimately discharge into surface watercourses, coastal waters and potentially into groundwater.
In addition to antimicrobials, their active compounds and resistant genes, the environment provides other drivers of resistance. This includes metals, which can promote mutations in microorganisms, biocides (surfactants and disinfectants), and microplastics, which can become a vehicle for the spread of resistant bacteria.
This is a global problem that affects not only human health but animal and environmental health and requires a multi-sector, ‘One Health’ approach to address it. We are already seeing this in the water cycle, with a number of wastewater treatment discharges upstream of raw water inlets for water treatment plants.
Why is antimicrobial resistance a problem and how can chemical engineers positively influence a solution for this issue?
The World Health Organization considers AMR to be one of the greatest human health threats. A report commissioned by the UK Prime Minister, published in 2016, predicted that, if we do nothing about it, AMR will be responsible for up to 10 million deaths per year globally by 2050 with over US$1 trillion in cumulative losses to the global economy.
In recent years there have been 1.27m deaths globally attributable to AMR. Antimicrobials underpin most of modern medicine including most surgery and chemotherapy treatment, without which, these are less safe. Without effective antimicrobials we can risk returning to a pre-antibiotic era where minor injuries could cause death through non-treatable infections.
Those outside the health sector may feel the issue can be resolved at the source – if we can develop new antimicrobials and get people to use them responsibly, this is all that is required. However, drivers of resistance are already widespread in the environment making this only part of a much wider solution. It requires a much broader multi-sector approach, and the water industry is also critical in this fight against AMR.
Within wastewater and treatment, we as chemical engineers must continue to examine treatment options, balancing this with a need to tackle AMR whilst managing costs. This is also the case for water treatment.
Understanding measurement and treatment of emerging contaminants will be key to reducing these risks in the future.
Sharing experience across the industry and looking at the research and evidence is the first step to solving this complex problem.
Tell us briefly about what is unique about your research/technology and how you feel it will make a positive difference to SD3: good health and wellbeing?
There is a growing body of research telling us where the likely global hot spots are for AMR emergence: places characterized by warm temperatures, low levels of sanitation coverage, and high levels of industrial pollution. We also know that whilst the use of antibiotics in health and agriculture varies hugely across the globe, the single factor that appears to have the strongest correlation with the risk of AMR transmission is infrastructure condition.
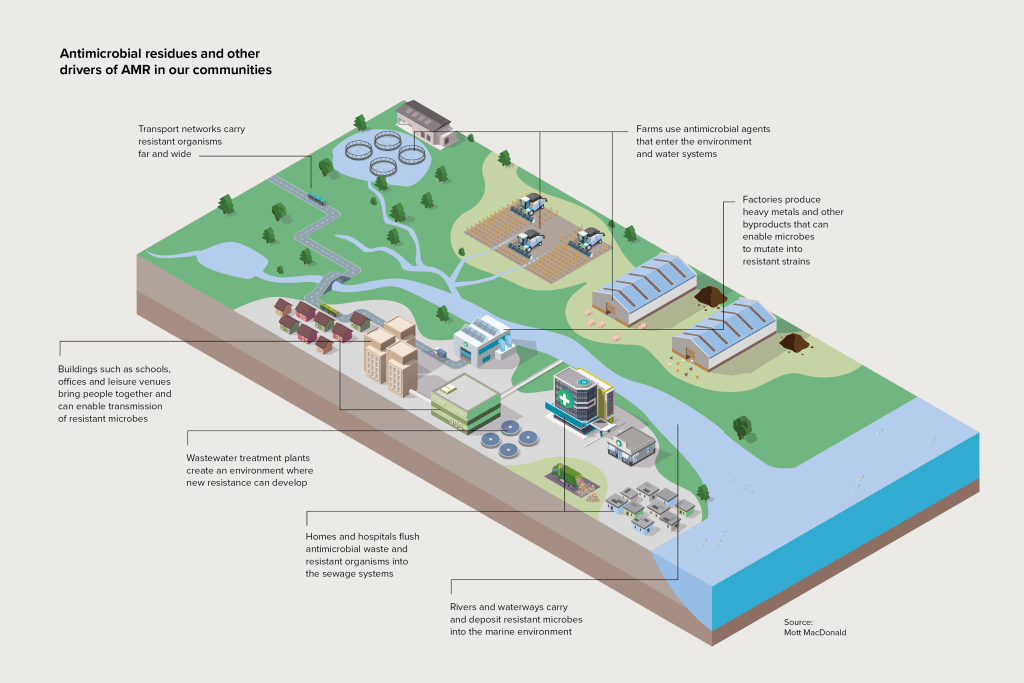
This is why Mott MacDonald is working globally to improve access to safe sanitation, and in more industrialised countries to reduce the frequency sewers discharge to rivers. As shown in Figure 1, AMR is a multicomponent problem reducing the adverse impacts will require collaboration with the various practices including: sustainability, climate change, buildings, water resources, as well as water and wastewater treatment.
We are empowering each of our practice leaders in these areas to address AMR in their projects and to work collectively. Strategic partnerships are being developed with academia, regulators and professional organisations.
Our approach is to embrace and champion the ‘One Health’ agenda.
Visit our Sustainability Hub to learn about others making a difference in our Sustainability success stories. There you can also access a suite of new on-demand training courses and knowledge resources to embed sustainable principles and practices into everyday work and life.